
Recently, a research team led by Professor Xu Qin from the School of Nursing at our university published a paper titled “Impact of the family cohesion-centered frailty intervention on older gastric cancer patients: a non-randomized controlled trial” in the international medical journal BMC Medicine (a top-tier journal in the first quartile of the Chinese Academy of Sciences classification, IF = 8.3).
This study explores a novel model of frailty intervention in older gastric cancer patients and achieves important progress by implementing interventions at the family level.
Frailty is a common geriatric syndrome among older gastric cancer patients, closely associated with adverse postoperative outcomes and significantly affecting recovery quality and long-term prognosis. Previous studies have largely focused on individual-level interventions such as nutritional support and exercise, while paying relatively limited attention to the role of the family in disease management. As survival among older gastric cancer patients improves, the setting of recovery is gradually shifting from hospital to home. As the most fundamental unit of social support, the family plays an irreplaceable role in promoting both physical and psychological recovery. Prior research by the team has also demonstrated that family cohesion is an important factor influencing frailty; however, intervention studies targeting this dimension remain scarce.
To address this gap, the team developed a family cohesion-centered frailty intervention program based on the Satir model of family therapy. The study adopted a non-randomized, time-sequence controlled trial design and was conducted at a tertiary hospital in Jiangsu Province. A total of 79 older gastric cancer patients at high risk of frailty, together with their family caregivers, were enrolled and assigned to either an intervention group (n = 40) or a control group (n = 39) according to admission time.
In addition to routine frailty management, the intervention group received a 4-week family cohesion intervention, including frailty-related health education, emotional recognition and regulation, exploration of personal resources, family communication training, and development of positive coping strategies. Data were collected at admission (T0), 4 weeks postoperatively (T1), and 1 month after the intervention (T2). Generalized Estimating Equations (GEE) were used to evaluate intervention effects.
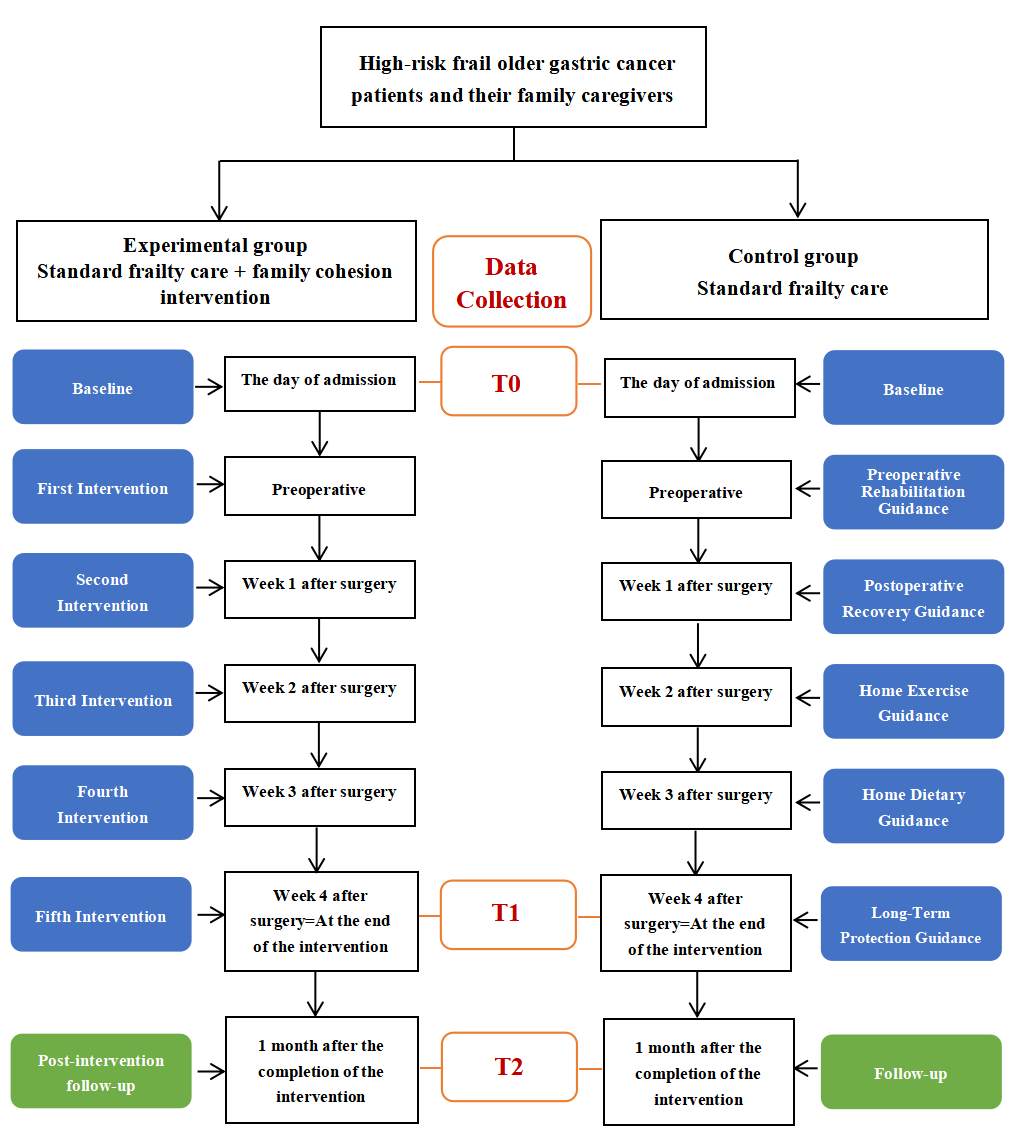
Fig 1. Intervention time and data collection flowchart
The results showed that, compared with routine care, the intervention group exhibited significant reductions in frailty levels, anxiety, and depression, as well as significant improvements in family cohesion, self-efficacy, and quality of life. The intervention effects became even more pronounced during follow-up. The interaction between group and time was statistically significant across outcomes. Sensitivity analyses produced consistent results, supporting the robustness of the findings. Although age, education level, and tumor stage showed some moderating effects, their overall influence was limited.
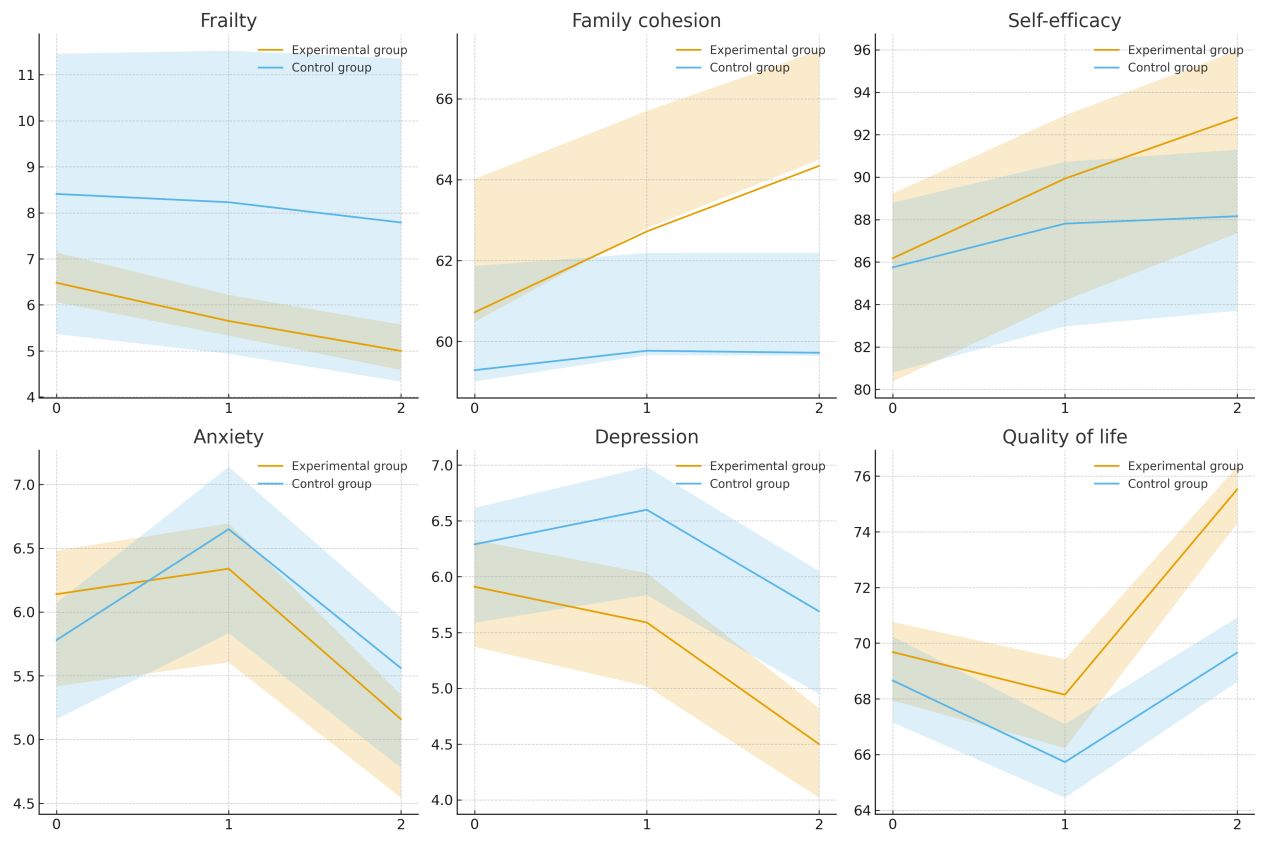
Fig.2 Estimated marginal means (MI-pooled GEE) for outcomes at different time points between groups
This study is the first to adopt family cohesion as the core intervention target and to systematically integrate the Satir Model into perioperative frailty management for gastric cancer patients. The findings demonstrate that family-level interventions can produce sustained improvements across physiological, psychological, and social dimensions. This research provides new theoretical insights and practical pathways for optimizing frailty management in older gastric cancer patients and offers strong evidence for developing family-participatory nursing models, with high potential for clinical application.
This work marks an important advance by the School of Nursing in the fields of oncology nursing and frailty intervention, highlighting the team’s innovative efforts in family-integrated care. Moving forward, the team plans to conduct randomized controlled studies and further promote the translation of these findings into clinical practice, with the aim of continuously improving health outcomes and quality of life for older gastric cancer patients.
Doctoral student Yinning Guo and master’s student Yimeng Chen are co-first authors of the paper, and Professor Xu Qin is the corresponding author. The study has been registered at the Chinese Clinical Trial Registry (ChiCTR2400082744) and was supported by grants from the National Natural Science Foundation of China (General Program No. 82073407 and Young Scientists Fund No. 72404140).
Full text link: https://doi.org/10.1186/s12916-026-04823-x
(Contributed by Xu Qin Research Group; Translation revised by Wu Wenbo)



